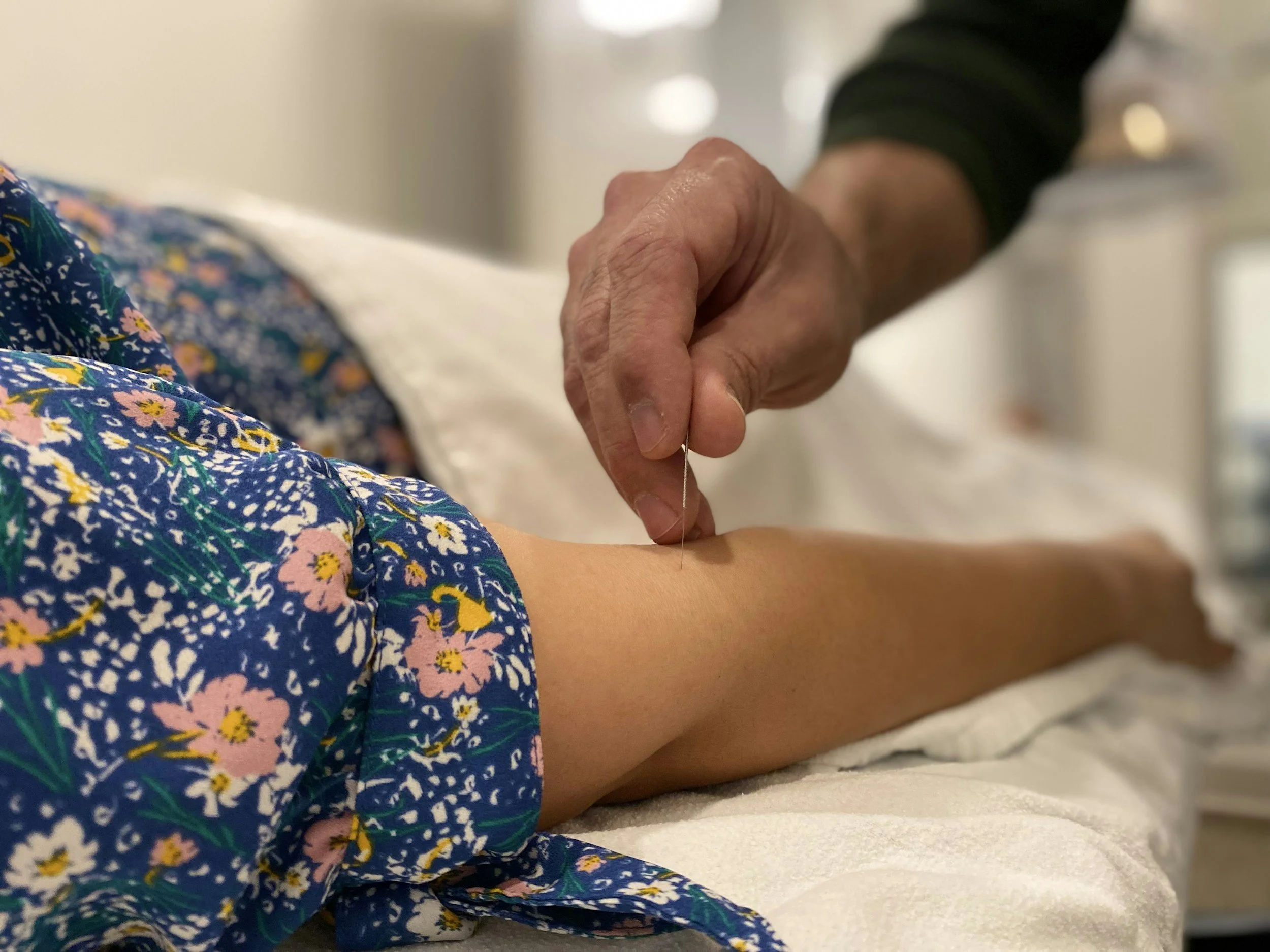
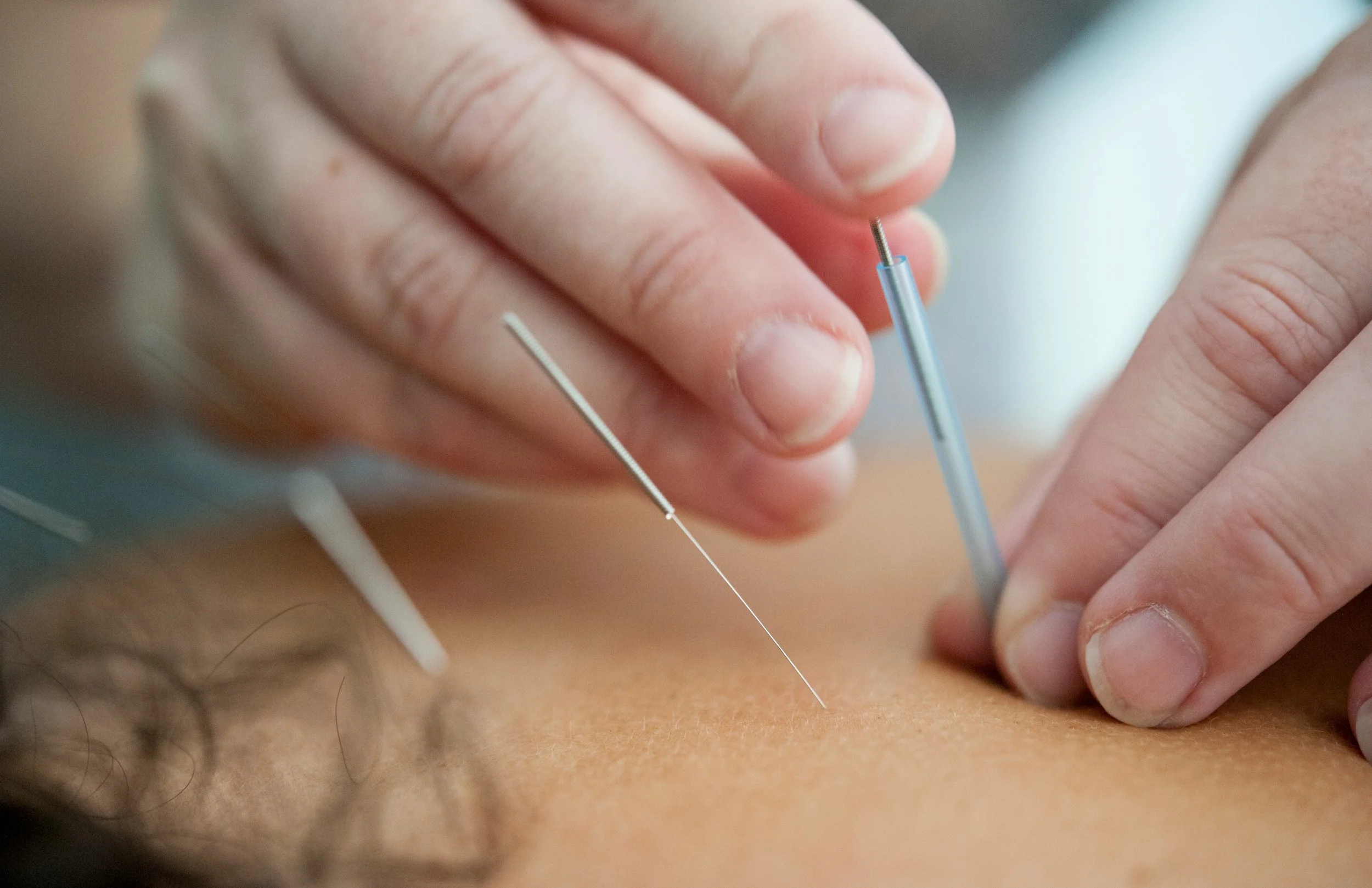
Acupuncture for Menopause
Menopause is a biological transition. The problem is not the transition itself. It is the symptoms.
Hot flashes that wake you at 3 a.m. Sleep that never feels restorative. Mood shifts that blindside you. Joint aches that show up out of nowhere. For many patients, these symptoms run for years.
This is one of the areas where acupuncture has meaningful clinical evidence. Not a cure, but a measurable reduction in the symptoms that disrupt daily life.
This page covers what acupuncture addresses during perimenopause and menopause, what a treatment course looks like, and where it fits alongside hormone therapy.
Who This Is Relevant For
You may benefit from acupuncture for menopause if:
Hot flashes or night sweats are waking you most nights, and daytime energy has collapsed
Your sleep pattern has changed, you fall asleep but wake at 2 or 3 a.m. and cannot go back down
Mood shifts, anxiety, or irritability showed up around your early 40s or after your last period
You have considered HRT but want to try something first, or your doctor has advised against it
You are already on HRT and still dealing with residual symptoms, or you want to reduce the dose
Joint aches, brain fog, or heart palpitations started alongside cycle changes
What Most People Get Wrong About Acupuncture for Menopause
"There is no real evidence. It is just placebo."
This is outdated. The Acupuncture in Menopause (AIM) study, a pragmatic randomised trial of 209 perimenopausal and postmenopausal women, found a 36.7% reduction in hot flash frequency at 6 months in the acupuncture group, compared to a 6% increase in the control group. Reductions persisted at 12 months after treatment ended. The ACOM study from Denmark found similar results after only five weekly sessions. The evidence is not perfect, and there is legitimate debate about sham acupuncture controls, but the claim that acupuncture does nothing for vasomotor symptoms is not supported by the literature.
"I will do one session and see."
One session is a diagnostic, not a treatment. Judging acupuncture on one visit is like judging a medication after one dose. The research protocols that show the strongest results use 5 to 20 sessions over 6 to 12 weeks. This matters for expectations from the start.
"It is either acupuncture or hormone therapy."
This is the wrong frame. For some women HRT is the right call. For others it is contraindicated due to breast cancer history, certain cardiovascular conditions, or personal preference. For many, a combined approach works best: HRT handles the hormonal floor, acupuncture addresses sleep, stress regulation, and residual symptoms.
What Acupuncture Actually Addresses During This Transition
Based on the clinical literature and what is seen in practice, acupuncture has the strongest effect on four symptom clusters.
1. Vasomotor symptoms (hot flashes and night sweats). This is the most studied outcome. Vasomotor symptoms affect 68 to 82% of women during the menopausal transition and are the most common reason women consider hormone therapy. Acupuncture appears to help by modulating autonomic nervous system activity and the hypothalamic-pituitary-adrenal axis, the system that also regulates the stress response. The treatment target is not just the flash itself. It is the regulatory system underneath.
2. Sleep disruption. This is where many patients see the earliest change. Before hot flashes reduce in frequency, they often reduce in intensity, meaning you wake but fall back asleep faster. Sleep quality typically improves within 3 to 5 sessions.
3. Mood, anxiety, and irritability. The hormonal fluctuations of perimenopause affect serotonin and GABA signalling. Acupuncture influences the same pathways indirectly through stress regulation. This is not a replacement for psychiatric care during a depressive episode. It is an adjunct. For the anxiety component specifically, see how acupuncture and TCM help with anxiety.
4. Joint pain and musculoskeletal aches. Less discussed but very common. Estrogen has anti-inflammatory effects, and its decline often shows up as new joint stiffness, frozen shoulder, or plantar fasciitis. Acupuncture for this pattern uses a different protocol from symptom-regulation points, which is why the treatment plan changes if joint pain is a primary concern. For broader pain patterns, see the approach used in chronic pain cases.
What acupuncture does not reliably address: accelerated bone loss, vaginal tissue changes like vaginal atrophy and dryness which usually need topical estrogen or specific products, and cardiovascular risk shifts. If these are your concerns, a GP or menopause specialist comes first. Acupuncture is an add-on, not a substitute.
Perimenopause vs Menopause: The Approach Is Different
These are two different phases, and they are not treated the same way.
Perimenopause can start in your late 30s and typically runs 4 to 10 years before your final period. Hormones are fluctuating wildly. Estrogen can be higher than normal one month and crash the next. The clinical picture is often irregular cycles, new PMS severity, sleep disruption, anxiety, and weight changes. Treatment focus: cycle regulation where possible, nervous system calming, and symptom management that adapts as hormones shift. Sessions are often more frequent early on, typically weekly for 4 to 6 weeks, then spaced out. For patients with irregular cycles as a primary concern, this overlaps with the approach used in acupuncture for menstrual health.
Menopause (12 months without a period) and postmenopause bring a more stable hormonal floor. Lower, but less variable. The symptoms are different: more persistent hot flashes, sustained sleep issues, joint aches, cognitive changes. Treatment focus: supporting the nervous system through sustained low estrogen, specific protocols for vasomotor symptoms, and maintenance spacing once you are stable.
A 43-year-old with irregular cycles and a 56-year-old five years post-menopause need different treatment plans.
What a Realistic Treatment Course Looks Like
Sessions 1 to 2: Detailed history, tongue and pulse diagnosis, treatment plan. The first two sessions are diagnostic as much as therapeutic. How your body responds informs the next phase.
Sessions 3 to 6: Core treatment phase. Most patients start noticing sleep changes or a reduction in hot flash intensity here. If nothing has shifted by session 6, the plan is reassessed. Point selection may need to change, or acupuncture may not be the right primary tool for your case.
Sessions 6 to 10: Consolidation. Symptoms that improved become more stable. Cupping or guasha may be added for joint pain, or food therapy recommendations for sleep and temperature regulation.
Maintenance: Once stable, spacing moves to every 2 to 4 weeks, then monthly, then as-needed.
Most of the clinical trial protocols referenced earlier used 10 to 20 sessions. In practice, 8 to 12 is the realistic target for meaningful, sustained change. Fewer if the case is straightforward. More if multiple overlapping issues are involved, for example menopause symptoms plus an old injury plus chronic stress.
For a framework on gauging whether treatment is working at each checkpoint, see how to tell if acupuncture is working.
Alongside HRT, Instead of HRT, or Neither
The decision about HRT is between you and your GP or menopause specialist. What can be said clearly:
If HRT is working well and you have no residual symptoms, acupuncture for menopause specifically is probably not needed
If HRT is working partially, which is common, acupuncture addresses residuals like sleep, joint pain, and anxiety without conflicting with the medication
If HRT is contraindicated or you have chosen not to take it, acupuncture is one of the non-hormonal options with reasonable evidence. Others your doctor may discuss include SSRIs, gabapentin, and cognitive behavioural therapy
If you are considering reducing your HRT dose, acupuncture can help soften symptom rebound during a taper. This should be coordinated with your prescribing physician
For support across the broader picture of hormonal and reproductive health including irregular cycles, PCOS, endometriosis, and fertility, see women's health and gynecological services. Related reading includes acupuncture for PCOS and acupuncture for fertility.
Who This Is For
Acupuncture for menopause may be a good fit if:
Symptoms are affecting sleep, work, or relationships and you want to address them
You want a non-pharmacological option, or you want to complement what you are already doing
You can commit to at least 6 to 8 sessions over 6 to 10 weeks to give the treatment a fair trial
You are comfortable with detailed questions about cycle, mood, sleep, digestion, and stress
Who It May Not Be For
It may not be a good fit if:
You are looking for a one-session fix
Your primary concern is bone density, vaginal atrophy, or a specific medical condition that needs a gynecologist
You have a needle phobia that cannot be managed with very thin needles and slow insertion
Act Now or Wait
Act now if: sleep has been disrupted for more than 4 weeks and it is affecting daytime function, mood or anxiety symptoms are new and escalating, hot flashes are interfering with work or social life, you are considering HRT and want to explore non-hormonal options first, or you are on HRT and still have significant residual symptoms.
You can wait if: you are in very early perimenopause with mild symptoms, you want to trial lifestyle changes first (sleep hygiene, exercise, caffeine and alcohol reduction, which do help), or you are stable and managing well.
Menopause is not an emergency. But chronic sleep loss has documented effects on cognition, cardiovascular risk, and mood, and symptomatic perimenopause can last a decade. Treating earlier usually means fewer sessions, because the nervous system has not become entrenched in dysregulated patterns.
How Neil Approaches Menopause Cases
Neil Dou is a Registered Acupuncturist with the College of Complementary Health Professionals of BC (CCHPBC) and Vice President of ATCMA. He has treated 7,000+ cases across Canada and China, with women's health forming a consistent part of that clinical workload. His background includes a Psychology degree from UBC alongside his TCM training at Kwantlen Polytechnic University, which informs how stress, sleep, and nervous system regulation are factored into menopause assessment alongside physical symptoms. Full credentials are on the About page.
Menopause treatment plans are run out of three locations across Greater Vancouver: Beyond Physiotherapy in South Surrey (Mondays), Beyond Physiotherapy in Langley (Saturdays), and BreakThru Kinetics in Surrey (Mondays, Wednesdays, and Fridays). Home visits are available for an additional fee.
Every menopause case starts with an assessment. What specifically is bothering you most, what you have already tried, what medications or supplements you are on, what your goals are. The assessment concludes with an honest read on whether acupuncture is likely to help and how many sessions to expect. If acupuncture is not the right primary tool for your case, that is said directly and alternatives are suggested.
Sessions run 45 to 60 minutes. Needles are sterile, disposable, and very thin. Most patients find the sessions deeply relaxing, and many fall asleep on the table, which is itself therapeutic for women dealing with chronic sleep disruption. Alongside acupuncture, food therapy, cupping therapy for joint aches, or guasha may be added depending on the presentation.
Direct billing is available with Pacific Blue Cross, Canada Life, Sun Life, and most major extended health providers.
Common Questions
How many acupuncture sessions are needed for menopause symptoms?
Most patients need 8 to 12 sessions over 8 to 12 weeks for meaningful, sustained change in vasomotor and sleep symptoms. Simpler cases may need fewer. Published trials that showed the strongest effects used 10 to 20 sessions. Some change should be noticeable by session 4 to 6. If not, the plan needs adjustment.
Does acupuncture work for hot flashes specifically?
The clinical evidence is suggestive, not definitive. The AIM study showed a 36.7% reduction in hot flash frequency at 6 months in the acupuncture group versus a 6% increase in the control group. Other trials have shown smaller effects. Practically, acupuncture is more likely to help than not, the side-effect profile is very low, but it is not a guarantee.
Can I do acupuncture if I am already on HRT?
Yes. Acupuncture does not interact with hormone therapy and can complement it. Many patients use acupuncture to address symptoms HRT does not fully resolve, commonly sleep, joint pain, and anxiety.
How is perimenopause acupuncture different from menopause acupuncture?
Perimenopause treatment often focuses on stabilising fluctuating hormones and regulating cycles alongside symptom management. Menopause treatment focuses on supporting the nervous system and organs under a sustained low-estrogen state. Point selection, treatment frequency, and adjunct therapies differ.
Is acupuncture covered by insurance in BC?
Most extended health plans in BC cover acupuncture performed by a Registered Acupuncturist. Coverage amounts vary significantly by plan. Check your specific policy for per-visit and annual limits.
What if I am needle-phobic?
Raise it at the assessment. Very thin, single-use needles (much thinner than injection needles) inserted slowly are tolerable for most needle-averse patients. For severe phobia, the approach starts with fewer points and builds up.
Are there side effects?
Serious complications are extremely rare with a Registered Acupuncturist. Mild side effects such as slight bruising at a needle site, brief tiredness after treatment, or occasional lightheadedness occur in a small number of cases and resolve quickly.
Book a Menopause Assessment
If you are in perimenopause or menopause and symptoms are affecting your life, the first step is an assessment.
It covers your specific symptom pattern, relevant history, and a clear treatment plan with a checkpoint at session 6. You will get honest answers on what to expect, what this can and cannot address, and a realistic session estimate.
Neil sees patients at clinics in Surrey, South Surrey, and Langley, with home visits available across Greater Vancouver.
Question before booking? Message at (604) 721-7984. Responses within 2 hours.
Neil Dou, R.Ac
Experienced & Trusted TCM Care
Registered Acupuncturist in BC with extensive clinical experience in both China and Canada.
Serving Richmond, Surrey & Greater Vancouver
Provides personalized acupuncture treatments and home visits across Richmond, Surrey, and Burnaby, recognized for effective care and positive patient feedback.
Proven Results With a Holistic Approach
With over 7,000 successful treatments, care focuses on pain relief, internal medicine, and long term healing through a holistic approach that combines acupuncture, food therapy, cupping, gua sha, and lifestyle guidance.